Tooth extractions, no matter what kind of teeth, can often carry the possibility of you developing a condition known as dry socket, also known as fibrinolytic osteitis or alveolar osteitis.
While some dry sockets can often heal soon enough if you take the necessary measures, several might need professional cleaning and treatment.
To learn more about what a dry socket looks like, along with some symptoms and risks that you might need to look out for, you can go through the following guide for easier identification.
When Do You Develop a Dry Socket?
Tooth extractions or other such dental surgeries that require an extraction can lead to the development of a dry socket.
Generally, whenever you have this kind of extraction, a blood clot will form on the site to help minimize the contact and exposure of the nerves and the bones to external elements that can include air, bacteria, food bits, and others.
This kind of blood clotting is essential so that the site of the surgery or extraction can heal quickly and effectively. However, if this blood clot cannot form or if it ends up getting displaced, then this is when a dry socket will form.
However, these kinds of dry sockets are quite rare when it comes to regular extractions, with only 1% to 5% of people experiencing them. However, if you have your mandibular third molar or wisdom tooth extracted, this rate can go beyond 30%.
This condition can lead to an infection and can be quite painful for up to five days. You should consult your dentist again to treat this condition.
What Does a Dry Socket Look Like?
If you examine the site of your tooth extraction or surgery carefully and notice a hole or cavity, this is most likely a dry socket. However, it might not always be easy for you to examine this site properly since dry sockets occur more frequently after tooth extractions of your molars and wisdom teeth, which tend to be situated at the back.
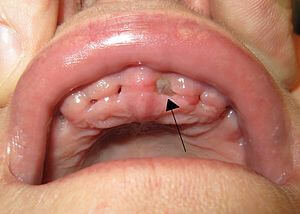
If there is no blood clot, it is quite likely that you have developed a dry socket. However, you should note that this dry socket can appear differently to different people depending on the kind and extent of the damage.
For instance, if the site appears hollow, but you can see your bone underneath and some dryness and whiteness around the area, these are signs of a dry socket.
In other cases, your dry socket might also end up looking dark and colored. If the site looks black, bluish, green, or yellow, this can suggest that an infection has already occurred due to the growth of bacteria. The presence of food bits can lead to this color as well.
In this kind of situation, it can be difficult to accurately recognize the site as a dry socket, so make sure you also get a diagnosis from your dentist.
Common Causes of a Dry Socket
Different people are likely to have different causes for this condition based on their habits and the nature of their extraction. However, some common reasons for a dry socket to occur are as follows.
- Food: If food particles keep getting stuck at the site and do not quickly dissolve, they can end up causing harm to the blood clot, displacing it from its position.
- Bacteria: Bacteria may grow and develop either due to the gathered food debris or other infections and exposures. These can increase the pain and affect the blood clot, leading to a dry socket that can appear blackish in color.
- Smoking: Smoking tobacco or nicotine can damage the natural mitigation process at the site of your surgery. The creation of healthy blood vessels can get affected, not to mention that the act of smoking itself can adversely affect the site due to the movements of your jaw and mouth.
- Pressure: There are many things we use our mouths for, such as chewing, biting, talking, sucking, or even clearing out your nose. This kind of pressure can end up displacing the blood clot, causing the dry socket to form due to prolonged exposure.
- Alcohol: Alcohol or any kind of soft drink can end up opening the blood clot and causing it to displace or dislodge. This is why it is essential to avoid alcohol or such drinks until the site heals and your dentist gives you the clear.
- Pills: If you are currently taking birth control pills, this too can alter your hormones and affect the blood clot at the site of the extracted tooth. The risk increases nearly twofold in this case, so make sure you time your surgery in a way that no interference can occur.
- Pre-existing Conditions: Pre-existing conditions can include cancer, diseases, sores, infections, and more. The presence of these conditions can increase the risk of patients developing a dry socket after tooth extraction.
- Traumatic Surgery: The kind of surgery that you had can itself become a cause for the occurrence of a dry socket. If it was particularly painful and difficult or there were some mistakes during the process, this could damage the natural growth of the blood clot, leading to the site’s exposure to several elements causing the dry socket.
Symptoms
Several symptoms can accompany a dry socket after your tooth extraction. It might be easy to dismiss some of these as normal after a tooth extraction or surgery, so make sure you look for a few of these symptoms occurring together so that you can figure out that something is wrong.
These symptoms can include the following.
- Pain at the site of extraction for up to five days following the surgery
- Strange or poor taste in the mouth
- Odor or foul breath
- Worsening or severe pain originating from the site and traveling to the eye and ear on the given side
- Fever
- Visible bone at the site of extraction
Risks to Watch Out For
There are several factors or habits that can lead to a greater risk of you developing a dry socket in your mouth. You can go through some of these below.
- Age: The older you are, the greater the risk of developing a painful dry socket. People more than 40 (sometimes even 30) years old might experience a dry socket considering that the jaw is more or less quite heavy with an insufficient supply of blood.
- Sex: Menstruating people or those who are on birth control might end up becoming more vulnerable to dry sockets due to the changes in the hormonal conditions.
- Smoking Habit: If you have a smoking habit or even an alcohol habit, you might be at greater risk of a dry socket after extraction due to the damage to the clot or simply an inability of the site to form a blood clot in the first place.
- Lack of Proper Hygiene: Dental and oral hygiene can help prevent dry sockets, but if you don’t regularly maintain this, the site might develop bacteria and increase the risks of a dry socket.
- Hormones: Taking hormones externally can also increase the risk of a dry socket, so make sure you figure out if you can pause these for some time surrounding your surgery or simply consult your dentist to prevent issues.
- Too Much Contact: Frequent contact such as making sucking movements, accidentally hitting the site, rinsing your mouth too much and too harshly or even overbrushing your teeth can put you at greater risk of a dry socket.
Treatment
You should immediately visit your dentist if you notice the signs of a dry socket so that they can help you treat the condition well. Your dentist will clean out the area, remove the socket and apply a dressing to the area that can help facilitate healing.
Following this, you will most likely need to extend the care and caution at home by taking some medicines, following a dental hygiene routine, and any other steps that your dentist might ask you to follow.
Prevention
Some ways to prevent the development of a dry socket include:
- Maintaining proper dental and oral hygiene at all times
- Reducing the frequency with which you smoke and drink
- Providing all your health-related details to your dentist before the surgery
- Avoiding soft drinks and beverages until you fully recover
- Sticking to softer food and then gradually moving on to regular food consumption
- Taking some time to let your site heal naturally instead of trying to rush the process
- Following all the post-surgery instructions that your dentist recommends
Final Remarks
A dry socket looks like a hole or cavity where you got your tooth extracted. It can either be white, black or green in color and can also result in symptoms like pain, fever, foul breath, bad taste and more. If you notice any of these symptoms, it is essential for you to seek professional treatment or consult your dentist for home treatment.